For millions of women worldwide, the journey to an endometriosis diagnosis is a grueling marathon of chronic pain, dismissed symptoms, and medical frustration. On average, a woman suffering from endometriosis will wait between 8 to 12 years before receiving a definitive diagnosis. This delay allows the disease to progress, causing immense physical suffering and, in many cases, threatening a woman’s fertility.
However, a groundbreaking Phase 2 clinical trial recently published in The Lancet Obstetrics, Gynaecology & Women’s Health offers a massive beacon of hope. Researchers at the University of Oxford have successfully tested a non-invasive radioactive tracer that can literally illuminate the disease on a scanner, potentially ending the need for invasive diagnostic surgery.
At Humane Medical Assistance, we specialize in bridging the gap between international patients and the most advanced medical technologies available globally. Understanding this new non-invasive endometriosis test is crucial for women advocating for their reproductive health. Here is a deep dive into the science behind this breakthrough and what it could mean for the future of women’s healthcare.
The Diagnostic Blind Spot: Why Does Endometriosis Take So Long to Find?
To understand why this new imaging tool is revolutionary, we must first understand why the disease is so notoriously difficult to spot.
Endometriosis occurs when tissue similar to the lining of the uterus begins growing outside of it. This rogue tissue responds to the body’s monthly hormonal cycles, swelling and bleeding just like the uterine lining does. However, because this blood has nowhere to exit the body, it causes severe, chronic inflammation, intense scarring, and adhesions that can actually fuse internal organs together.
While the pain is undeniable, the physical evidence of the disease frequently evades doctors. Dr. Anshumala Shukla Kulkarni, a leading minimally invasive gynecologist, explains that the disease generally presents in three forms:
- Ovarian Endometriomas: These are cysts filled with old blood that are large enough to appear clearly on standard ultrasounds.
- Deep Infiltrative Endometriosis: This severe form invades other organs and can usually be spotted using transvaginal ultrasounds or MRIs.
- Superficial Peritoneal Endometriosis (SPE): This is the diagnostic nightmare. SPE consists of tiny lesions scattered across the pelvic lining. They are incredibly small—sometimes just 3 to 4 millimeters—making them completely invisible to conventional imaging tools like ultrasounds and MRIs.
The tragic reality is that SPE accounts for 80% of all laparoscopically diagnosed cases, making it the most prevalent form of the disease. Because their scans come back “clear,” patients with SPE are frequently misdiagnosed with stress or Polycystic Ovarian Disease (PCOD) while their endometriosis continues to aggressively advance.
Until now, the only way to definitively prove the existence of SPE was to put the patient under general anesthesia and perform a diagnostic laparoscopy—an invasive abdominal surgery.
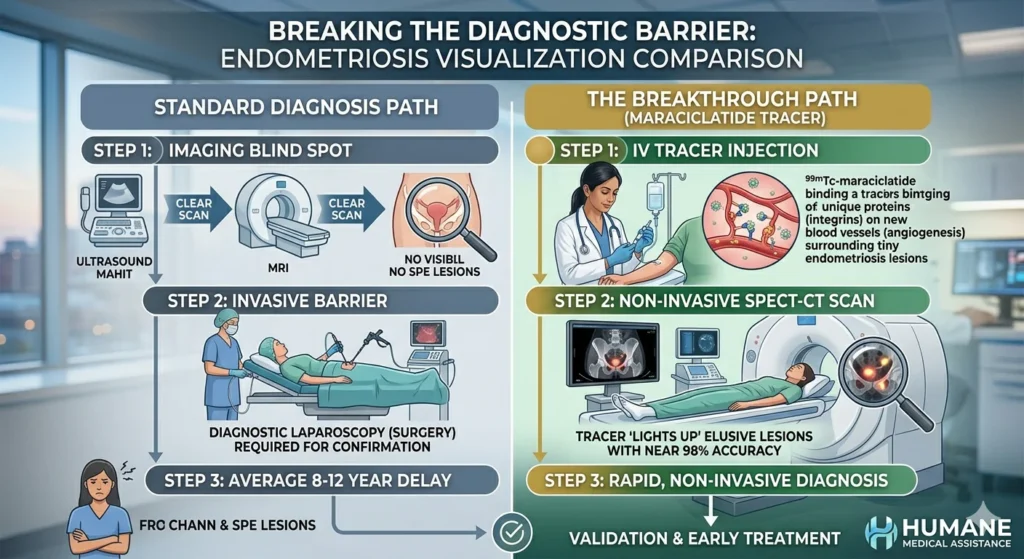
Lighting Up the Invisible: How the Radioactive Tracer Works
The Oxford study targets this exact diagnostic blind spot using a highly specialized molecular imaging agent called 99mTc-maraciclatide.
Here is how this revolutionary non-invasive endometriosis test works:
- Targeting Angiogenesis: As endometriosis lesions grow, they demand a blood supply. They release signals that cause new blood vessels to form around them, a process known as angiogenesis. These new vessels are packed with high levels of specific proteins called integrins.
- The Radioactive Dye: Maraciclatide is a dye-like tracer that is specifically engineered to bind to these exact integrin proteins.
- The Scan: The patient receives the tracer intravenously. The radioactive dye travels through the bloodstream, seeking out and concentrating within the blood-rich endometriosis lesions.
- The Result: The patient then undergoes a SPECT-CT scan (a highly detailed imaging test). The scanner detects the concentrated radioactive dye, causing the previously “invisible” lesions to light up vividly on the monitor.
The Phase 2 trial results were spectacular. The tracer correctly identified the disease in 14 out of 17 surgically confirmed cases, including the tiny, elusive SPE lesions that prior ultrasounds and MRIs had completely missed. Furthermore, it produced zero false positives, proving to be a highly reliable diagnostic tool.
What This Means for the Future of Women’s Health
While the technology is still in early clinical phases and awaits full regulatory approval, its potential impact on endometriosis management is seismic.
1. Ending the Cycle of Doubt Perhaps the most significant benefit is validation. Dr. Kulkarni notes that young patients suffering from severe symptoms often face skepticism from doctors and family members because their standard scans are clear. Without visual proof, families hesitate to start necessary hormonal therapies, allowing the disease to worsen. A scan that definitively proves the presence of the disease removes this doubt, empowering patients to seek immediate, aggressive treatment.
2. Preserving Fertility Endometriosis is a progressive disease. If allowed to advance unchecked for a decade, it can severely damage a woman’s reproductive organs. Catching the disease in its earliest stages using a simple, non-invasive scan allows doctors to initiate therapies immediately, potentially preventing the irreversible damage that leads to infertility.
3. Precision Surgical Planning Currently, when a surgeon performs a diagnostic laparoscopy, they often do not know exactly where the lesions are located until they are already inside the abdomen. If the maraciclatide tracer maps the exact location and spread of the disease beforehand, surgeons can plan much safer, more targeted, and highly efficient excision surgeries.

Navigating Advanced Diagnostics with Humane Medical Assistance
The global medical community is watching this technology closely as it enters Phase 3 international trials later this year. If successful, this radioactive tracer will fundamentally rewrite the global standard of care for endometriosis diagnostics.
At Humane Medical Assistance, we recognize that waiting for local healthcare systems to adopt advanced technologies can be agonizing, especially when you are living with chronic pain. We operate as a dedicated medical facilitation agency, connecting international patients with the premier global institutions leading these clinical advancements.
How We Facilitate Your Care:
- Global Connections: We maintain robust networks with top-tier international gynecological centers and research hospitals at the forefront of endometriosis innovation.
- Expert Second Opinions: We facilitate remote consultations with leading global specialists who can review your complex medical history and advise if you are a candidate for advanced diagnostic trials or specialized excision surgeries.
- Seamless Logistics: If you choose to travel for international medical care, our team handles every detail—from medical visas and specialized flights to on-the-ground care coordination—ensuring your journey is completely stress-free.
You do not have to accept a decade of suffering as normal. As medical science rapidly advances, Humane Medical Assistance is here to ensure you have access to the absolute highest standard of global healthcare, empowering you to reclaim your health and your life.

